Pleural disorders
Pleural disorders refer to conditions affecting the pleura, a double-layered membrane surrounding the lungs. The pleura plays a crucial role in protecting the lungs and allowing smooth lung movement during respiration. Disorders of the pleura can cause pain, difficulty breathing, and other respiratory complications. Some common pleural disorders include pleuritis (pleurisy), pleural effusion, and pneumothorax.
1. Pleuritis (Pleurisy)
Pleuritis is the inflammation of the pleura, which often results from an infection, such as pneumonia, or from an underlying medical condition like autoimmune diseases (e.g., lupus or rheumatoid arthritis). When the pleura becomes inflamed, the layers rub against each other, causing sharp chest pain, especially during breathing or coughing. The pain can be localized to one side of the chest and may worsen with deep breaths or movement. Other symptoms may include shortness of breath, coughing, and fever, depending on the underlying cause. Treatment focuses on relieving pain and inflammation, often with anti-inflammatory medications like NSAIDs (nonsteroidal anti-inflammatory drugs) or corticosteroids. If an infection is the cause, antibiotics or antiviral medications may be required.
2. Pleural Effusion
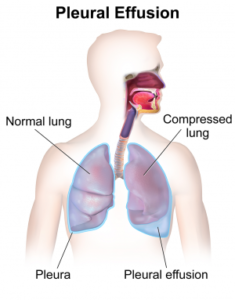
Pleural effusion is the accumulation of excess fluid in the pleural space between the pleura and the lungs. This fluid can be caused by various conditions, such as heart failure, pneumonia, tuberculosis, cancer, or kidney disease. The buildup of fluid can compress the lungs, making it difficult to breathe and leading to symptoms like chest pain, coughing, shortness of breath, and in severe cases, decreased breath sounds. Pleural effusion is diagnosed with imaging tests, such as a chest X-ray or ultrasound, and sometimes a thoracentesis procedure (inserting a needle to remove fluid) is performed to analyze the fluid and determine the underlying cause. Treatment depends on the cause and severity of the effusion. In some cases, draining the fluid through thoracentesis or placing a chest tube may be necessary. If the effusion is due to an infection or malignancy, specific treatments like antibiotics, chemotherapy, or radiation may be required.
3. Pneumothorax
Pneumothorax refers to the presence of air in the pleural space, causing the lung to collapse partially or fully. This condition can occur spontaneously, particularly in people with lung diseases like emphysema or asthma, or as a result of trauma, such as a rib fracture or a puncture wound. A pneumothorax may also develop after medical procedures like a biopsy or mechanical ventilation. Symptoms of pneumothorax include sudden chest pain and difficulty breathing. In severe cases, it can cause hypoxia (low oxygen levels) and shock. Treatment for pneumothorax depends on its size and severity. Small pneumothoraxes may resolve on their own, but larger or symptomatic cases may require the removal of air through a needle or chest tube. In some cases, surgery may be needed to prevent recurrence.
4. Hemothorax
Hemothorax is a condition where blood accumulates in the pleural space, often due to trauma, such as a chest injury or surgery, or from complications of certain diseases (e.g., cancer or blood clotting disorders). The symptoms are similar to those of pleural effusion, with chest pain, difficulty breathing, and decreased breath sounds. Hemothorax is typically diagnosed through imaging, such as a chest X-ray or CT scan. Treatment often involves draining the blood through a chest tube or, in severe cases, surgery to stop the bleeding and remove the blood.
5. Pleural Mesothelioma
Pleural mesothelioma is a rare but aggressive cancer that develops in the pleura, often as a result of long-term asbestos exposure. This cancer can cause pleural thickening, fluid buildup, and other complications. Symptoms include chest pain, difficulty breathing, and fatigue. Treatment may involve surgery, chemotherapy, and radiation, but the prognosis is generally poor, as the disease is often diagnosed in its advanced stages.
Conclusion
Pleural disorders can significantly affect respiratory function and quality of life. Early diagnosis and appropriate treatment are essential for managing these conditions effectively. Depending on the cause and severity, treatments may involve medications, drainage procedures, surgery, or supportive care to relieve symptoms and prevent complications. Regular follow-ups and management strategies are crucial, especially for chronic or recurrent pleural conditions.
